The Sickbay™ Platform
The only vendor neutral, FDA cleared SaaS platform to unlock time-series waveform data to enable flexible, centralized remote monitoring of any bed and the development and deployment of real-time AI in a standardized workflow from hospital to home.
With the Sickbay™ Platform
The only vendor neutral, FDA cleared SaaS platform to unlock time-series waveform data to enable flexible, centralized remote monitoring of any bed and the development and deployment of real-time AI in a standardized workflow from hospital to home
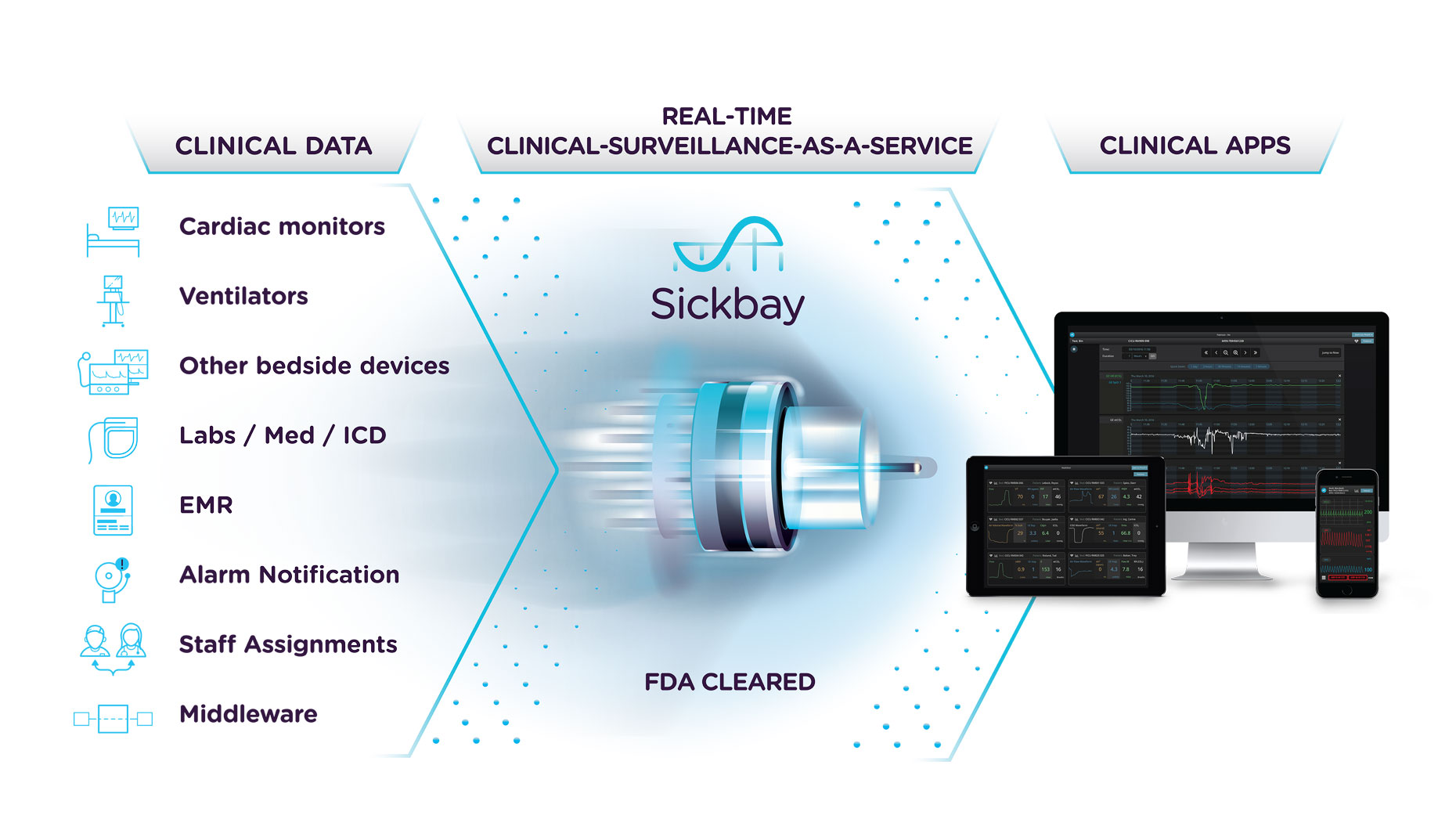
Sickbay™ Apps to Support Virtual Care and Remote Monitoring Workflows
Individual Apps
The Sickbay™ platform is giving hospitals the ability to rapidly scale any bed to a monitored ICU bed within minutes through a simple database change, across units and vendors. Facilities are also using the platform and data to create other flexible remote command centers for ventilator management, SpO2, and/or telemetry monitoring along with user configurable acuity scoring to better triage and manage patient deterioration.
Below are the applications that are typically deployed to support these remote monitoring workflows, to support the pandemic and create the foundation for a new standard of software based monitoring and data driven care.
MultiMon
Enable virtual rounding in weeks — not months — and extend bed capacity in minutes to transform any bed into a monitored ICU bed.
PatMon
Visualize monitor and ventilator data outside of the room, integrated in a single view, limiting unnecessary use of PPE.
Patient Hx
Automatically build beat-to-beat trends for an entire length of stay, with integrated vent data, to give providers the data they need to intervene faster.
Risk Score Calculator
Leverage unlimited retrospective data to create real-time risk calculators, virtual rounding reports, and patient-specific analytics to help avoid intubation and manage ventilated patients better.
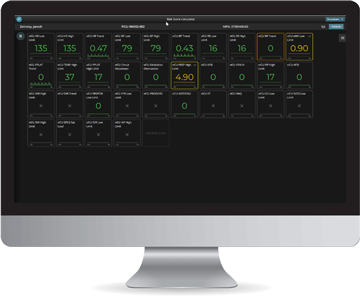
Two of the key benefits the combined solution enables in addition to the above include:
Create Flexible, Vendor-Agnostic vICUs and Command Centers
Combine all applications to create virtual ICUs and telemetry, ventilator, SpO2, or other command centers that can monitor up to 100 patients across units, facilities and vendors.
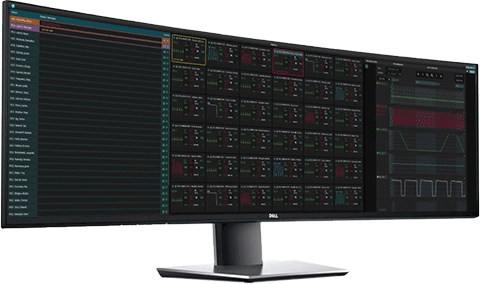
Extend Virtual Rounding and Mentoring
Give any provider, nurse, or other member of the healthcare team the ability to monitor patients and/or mentor and support bedside staff from a conference room, office, or home with access to all near real-time and retrospective data PC’s, tablet or phone to help manage staff shortages, get more eyes on patients, and expedite care and intervention.
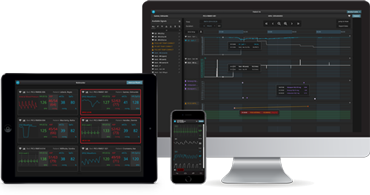

Featured Apps & Use Cases
Sickbay™ features web-based applications that transform data into actionable information to help care teams make better, faster decisions, and save lives.
Move your mouse over a card below to learn more.PatMon
Access real-time waveforms for remote viewing, command centers, and phone integration
MultiMon
Create vICUs, Virtual ICU
patient watch lists, and more for multiple patients - across vendors, units, and facilities
Patient Hx
View patient history including vitals and waveforms from 1 second to 1 year on your PC, tablet, or phone
Patient Hx with Strip Export
Automatically send ECG Electrocardiogram
strips and full trends to your EMR
Alarm Manager
Quickly meet NPSGNational Patient Safety Goals goals, automatically track KPI’s Key Performance Indicatorsacross all monitored patients, and reduce alarm noise at the source
PatMons Alarms
Optimize alarm limits in 2 minutes or less for individual patients
Risk Score Calculator
Expedite the calculation of common risk scores to decrease patient risk
Rapid Research
Triple your research grant output by manipulating and viewing data on the fly using standard development tools
It's time to create a new standard of care.
It's time to break down the data silos from proprietary vendor formats.
It's time to move from hardware-based to software-based monitoring.
It's time to unlock patient data from the bedside so more lives can be saved today and create a new standard of care for tomorrow.
We are here to help.